What a Good Lipoedema Assessment Looks Like

If you’ve spent years searching for answers about pain or changes in body shape, you deserve an assessment that truly listens. For too many people with lipoedema, the path to diagnosis has been long, confusing, and emotionally draining.
At Accelerate CIC, our clinicians specialise in complex chronic conditions including lipoedema, lymphoedema, and venous disease. We believe that a good assessment should feel unhurried, comprehensive, and validating – because understanding what’s really happening is the first step toward relief.
Step 1: Your History Matters
A good assessment begins with your story.
We explore when your symptoms began, how they’ve changed, and what makes them better or worse.
Key points we discuss include:
- Onset and progression: Did symptoms begin around puberty, pregnancy, or menopause? Have they got worse?
- Past medical and surgical history and medication taken
- Pain and tenderness: are your legs sore or sensitive to touch?
- Daily variation: Do symptoms change with heat, hormones, or time spent standing?
- Family history: Has anyone else experienced similar symptoms?
- Sudden changes: Rapid swelling or new pain may suggest another condition that needs ruling out.
These questions help us understand not only your physical symptoms but also their pattern over time – a crucial clue in differentiating lipoedema from other conditions.
Step 2: Focused Examination
The physical examination is a cornerstone of establishing an accurate diagnosis.
Your clinician will look at:
- Extent and shape: Lipoedema typically causes symmetrical enlargement of the legs or arms, often sparing the feet and hands.
- Tenderness: Lipoedema means that your legs or arms may be tender, painful or sore, unlike standard fat accumulation.
- Skin changes: While the skin usually looks normal, there may be a soft, dimpled (“cellulite-like”) texture.
- Function: How you walk and move matters. Lipoedema can alter the way you walk or place extra strain on joints and soft tissues, so we assess your gait and biomechanics
This part of the process helps confirm whether the features match the pattern of lipoedema or suggest another cause.
Step 3: Standardised Measurements and Imaging (When Needed)
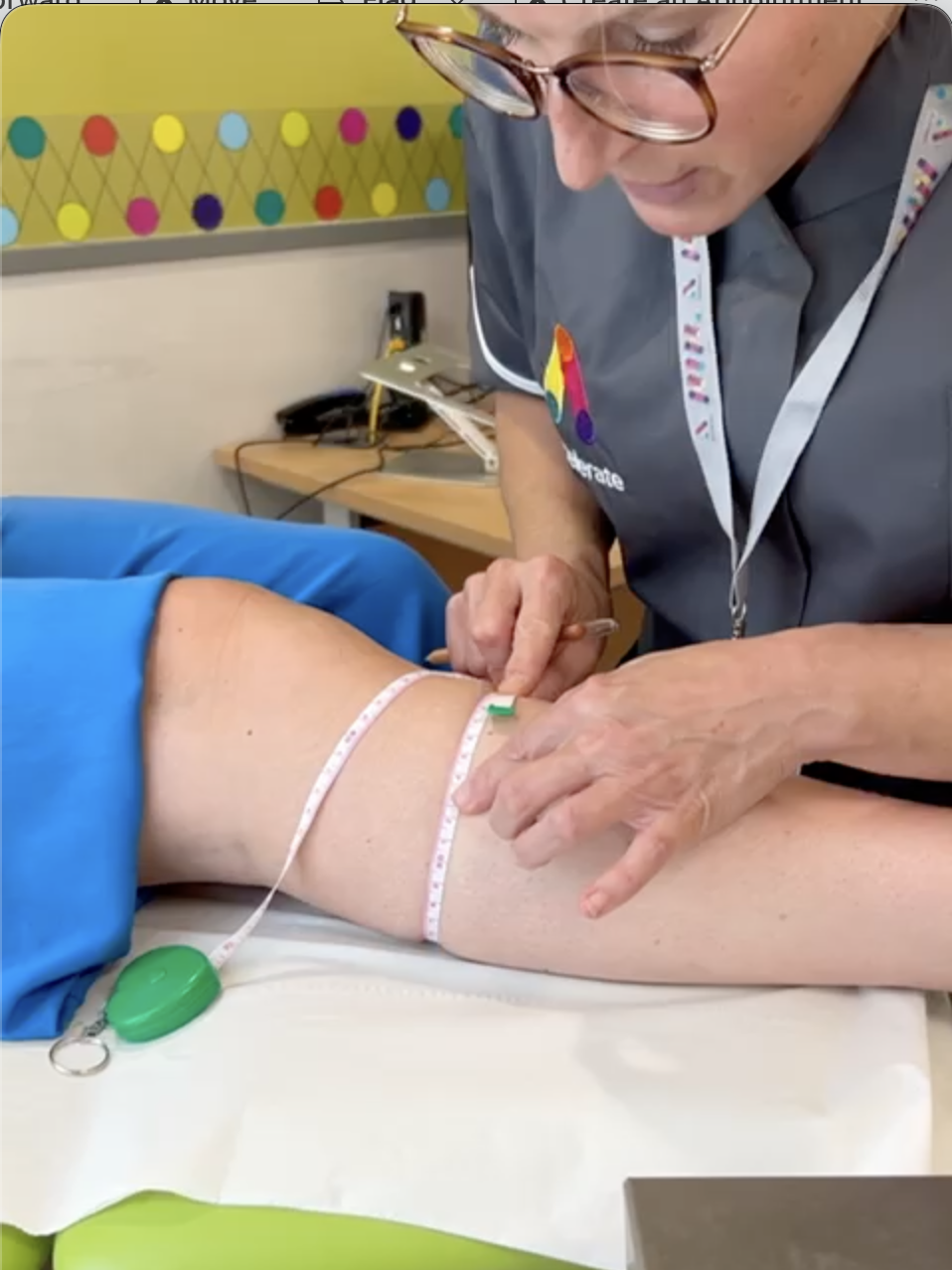
A reliable baseline helps us track progress and measure change. We take limb circumference measurements at standard points such as the ankle, calf, knee, and thigh.
While there’s no single test that “proves” lipoedema, specialist tools can support diagnosis and exclude other conditions. For example, a Tissue Dielectric Constant (TDC) moisture meter measures water content in the tissue, helping to identify whether lymphoedema (fluid-based swelling) is also present.
Imaging such as ultrasound or venous duplex scanning may occasionally be requested via your GP to rule out deep vein thrombosis (DVT) or chronic venous disease, but they’re not required to diagnose lipoedema.
Step 4: Considering Differential Diagnoses
Lipoedema can resemble several other conditions, so part of a good assessment involves considering what else it could be. These include:
- Lymphoedema – lymphatic failure, resulting in swelling, skin and tissue changes and a predisposition to infection. Chronic venous disease – skin and tissue changes related to underlying vein problems, e.g. haemosiderin staining or varicose veins.
- Lipohypertrophy – symmetrical fat distribution without pain or bruising.
- General adiposity – weight gain that follows a more proportional pattern.
An experienced clinician can distinguish these through pattern recognition, palpation, and detailed clinical reasoning.
Step 5: Creating a Personalised Plan
By the end of a specialist assessment, you should have an individualised and explicit, evidence-based plan for managing your condition.
This may include:
- Professionally fitted compression garments that support and shape comfortably.
- Guidance on movement and activity – safe, achievable routines that improve function without increasing pain.
- Skin care routines to protect and maintain skin health.
- Where appropriate, support for footwear and orthotic adjustments to improve comfort and mobility.
- Support with your well-being and, where necessary, referral for mental health care.
At Accelerate, we believe this plan should empower you to take control of your symptoms, not leave you feeling overwhelmed. We also communicate directly with your GP so that your ongoing care remains coordinated and informed.
What to Expect at Accelerate CIC
A typical private consultation lasts around 60–75 minutes, allowing you time to discuss your concerns and symptoms, examination, measurement, and care planning.
A follow-up appointment is often recommended in 6–12 weeks to review comfort, wear time, and progress.
Our aim is that everyone leaves their first visit with a clear diagnosis and a practical management plan – often after years of uncertainty elsewhere.

Find Expert Support
At Accelerate CIC, our team specialises in the diagnosis and management of lipoedema and lymphoedema. We’re proud partners of national organisations including the British Lymphology Society, Lipoedema UK, Lymphoedema Support Network, and Lymphoedema United, helping shape best practice across the UK.
